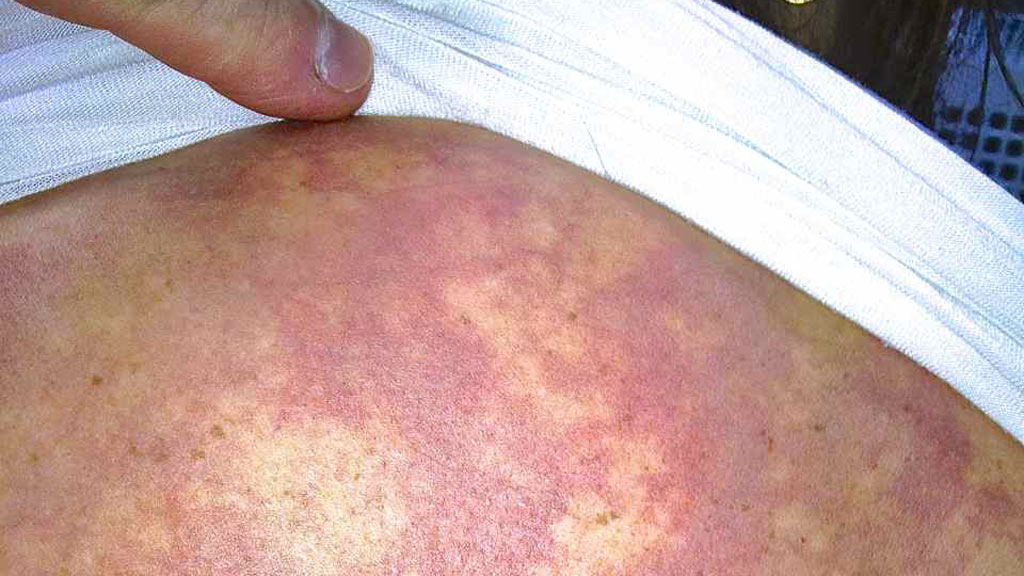
Incident Assessment: Skin Bends
In this incident, a diver in Indonesia experiences a skin rash post-diving for the second time in 6-months.
A 35-year-old female diver with 283 lifetime dives called the DAN Diving Emergency Service (DES) Hotline with skin symptoms. She was on the first day of her trip in Lembeh. She had completed three dives all to around 24m for 65 minutes with surface intervals of 1:45 and 2:10. All dives were on air with no decompression required.
Onset of Symptoms
Two hours post-diving she felt tenderness on her right thigh and noted a rash on her upper leg and torso. Three hours post-diving the rash had a bruise-like appearance and she had commenced breathing oxygen.
The diver advised DAN that she had a similar episode in February, which resolved by breathing oxygen.
Treatment
DAN recommended that she breathe oxygen for 3-hours and then the DAN diving doctor would re-assess her symptoms. DAN was advised that all the symptoms had resolved after 45 minutes of breathing oxygen, but she remained on oxygen for the full 3-hours DAN recommended. This was provided via a non-rebreather mask at 15 litres per minute.
That evening, she had dinner, drank plenty of water and went to bed. The Dive Operator’s staff checked on her a couple of times throughout the night and she was sleeping soundly. Symptoms did not return the following day.
The Member was advised not to fly for 72 hours from the resolution of symptoms. If symptoms returned she was asked to contact DAN immediately upon arriving home to Singapore, so evaluation/treatment could be arranged, but this was not required. However, a follow-up with a diving doctor was still recommended prior to diving again.
Diagnosis: Decompression sickness (DCS)
ADVICE: Given the Member experienced a similar skin-related bend in February, the possibility of the Member having a PFO was discussed and she was encouraged to undergo testing.
A post-dive change in the colour or texture of your skin, such as a rash or a marbled appearance, with or without an itch, may be decompression-related. Skin manifestations of DCS, also known as cutaneous DCS, are more common than you might think.
Divers often mistake cutaneous DCS for a rash due to another cause, such as contact with marine life or an allergic reaction, or they may just ignore such symptoms. Although cutaneous DCS in itself is usually a mild and self-limiting disease, the rash is often associated with neurological changes, which may sometimes be subtle. A diving medical specialist should be consulted promptly to assess the situation. This can be done a DAN-supported hotline.
Onset and Evolution
DCS-related skin changes usually occur within several minutes to several hours after a dive. The more severe your dive exposure, the more quickly symptoms are likely to be evident.
- An Itch: Is usually the first symptom to go away.
- A Rash: May resolve within 24 hours.
- Marbling: Usually fades out over a few days and never changes colour to blue-green, as a bruise does.
- Lymphatic DCS: May go away on its own, but both marbling and swelling will disappear more quickly with treatment.
In fact, with prompt and appropriate oxygen first aid for a sufficient duration (usually 4 hours is recommended), the rash and other symptoms can disappear and not recur. However, if the oxygen first aid is poor and/or stopped too soon, symptoms may persist or come back again.
Risk factors
The main risk factor for cutaneous DCS is your dive profile (e.g., multiple repetitive dives with relatively short surface intervals (often 1-2 hours)); however, divers with a large patent foramen ovale (PFO) – a fairly common, congenital, generally benign hole between the heart’s left and right chambers— may be at increased risk. A history of repeated cutaneous DCS (as in this case) or of DCS accompanied by other symptoms frequently leads to identification of a previously unsuspected PFO.
Treatment
Any skin change that might be DCS-related should be evaluated by a physician. A rash unaccompanied by other symptoms usually doesn’t need to be treated by recompression. But if your physician discovers signs of neurological effects, hyperbaric oxygen treatment in a recompression chamber is usually advised. Appropriate treatment for skin mottling or swelling will depend on the results of a physical examination. Skin changes associated with any other manifestations of DCS should be treated as an emergency.
Emergency Warnings
Abdominal, back or chest pain accompanied by skin mottling can quickly evolve into severe DCS and should be treated on an emergency basis. The shorter the time between a dive and the onset of symptoms, the more likely it is that severe DCS will develop.
First Aid
In all cases call the DAN Diving Emergency Hotline promptly for advice.
READ MORE ‘Fast Facts about Skin Bends’, including images of the various types of skin rashes.