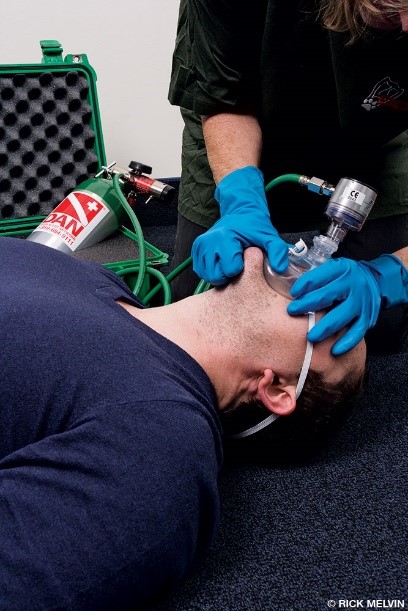
Symptoms do not always point to just one definite cause, so it is often just as important to continue listening to the patient and exploring options that might not be immediately apparent.

The Diver
The diver, a 32-year-old male, was an experienced recreational dive instructor. Approximately 18 months prior to the dive incident, he was injured in an all-terrain vehicle accident, suffering serious injuries to his face and skull. He required multiple surgeries to repair and reconstruct the orbit of his left eye, both zygomatic arches (cheek bones) and his maxilla (upper jaw). Some of the fractures entered the maxillary sinus cavity. The diver’s maxillofacial surgeon authorised him to return to diving after a prolonged recovery. He gradually resumed diving with no problems or complications.
The Dive
The diver was instructing a class of four students for their second day of open-water dives. The dive was planned with a beach entry and a brief surface swim to an area with a maximum depth of 9mt, accompanied by a certified divemaster and an experienced rescue diver. When the group began to descend, the instructor immediately experienced intense pain on the left side of his face from his cheek to his forehead. The pain quickly progressed from distracting to incapacitating.
The divemaster recognised that the instructor was having a serious problem and safely ascended with the students from about 5m. The rescue diver descended to assist the instructor, finding him on the bottom holding the left side of his face with one hand and securing his regulator in his mouth with the other. The rescue diver was able to assist the instructor in making a controlled ascent to the surface. They established positive buoyancy and reached shore. The pain was so severe that the divemaster called emergency medical services (EMS) and waited for an ambulance to arrive. The EMS crew performed a quick assessment and transported the instructor to the closest emergency department (ED), which was at the hospital where he had been treated for his previous injuries.
Medical Evaluation
The ED staff administered pain-relief medication. The attending physician examined the diver and promptly sent him for a CT scan of the head and face. Consulting the scans, the attending radiologist and maxillofacial surgeon who had previously treated him found no obvious signs of complications associated with the surgeries. The sinuses, orbit and other bones were healed, and no hardware had been displaced. There was no clear cause of the intense pain. The doctor prescribed pain medication and scheduled a follow-up appointment for the diver to see the maxillofacial surgeon.
The next day the diver called the DAN® Medical Information Line (+1-919-684-2948) and told the DAN medical staff about his experience. Because the most likely cause of his symptoms was a complication from his previous injuries, the caller sought a referral to an ear, nose and throat (ENT) specialist with dive medicine experience. Fortunately, a suitable ENT in the DAN referral network was near his home. The specialist, who also suspected a complication from the diver’s previous injuries, could not offer a solution other than to continue taking the medication and following up with his surgeon. Ten days after the dive, his pain persisted and was relieved only by the medication.
A Different Perspective
Despite the pain, the diver kept a scheduled appointment with his dentist for an unrelated issue. During the examination the dentist was able to localise the pain in an upper bicuspid (tooth between the canine and molar). After taking X-rays, the dentist determined that the root of the tooth had an abscess and the tooth was cracked. It is likely that during equalisation the diver unintentionally forced food, air or some other material into the tooth, which prompted pain associated with the exposed nerve. The dentist extracted the tooth, and there was purulent drainage from the socket, which is a sign of infection. The pain subsided as the fluid drained. By that evening the diver no longer needed to take pain medication, only an antibiotic to address the infection.
Conclusion
This case is an example of how easily prior medical history can become a focal point. A history of severe injury certainly warrants an evaluation of the previously affected areas, but this focus should not happen at the exclusion of other possibilities. The doctors, the specialist and DAN medics all lost objectivity to the physical discomfort of the patient. Fortunately, his situation was not life-threatening, although he required pain medication longer than he would have with a more thorough evaluation. It is imperative to try to avoid opiate use for any longer than necessary.
Every misstep is a teachable moment: All of us in DAN Medical Services learned from this case to remain diligent in our evaluations and avoid tunnel vision.
© Alert Diver — Q4 Fall 2018